Swedish Architecture firm, White Architects recently unveiled their design for a new mother and baby unit for the Panzi Hospital in the Democratic Republic of Congo.
The firm developed a new facility to be integrated into the existing hospital, designed to improve the wellbeing for mothers and children. The project, which was entered into the Africa Architecture Awards back in 2017, features a number of sustainable design strategies, much of which is covered in this comprehensive report by the firm.
PROJECT DESCRIPTION
Panzi General Referral Hospital is situated in the Ibanda Health Zone in Bukavu, Democratic Republic of Congo. Founded in 1999 by Dr Mukwege, it was planned for 120 beds, but currently has 450.
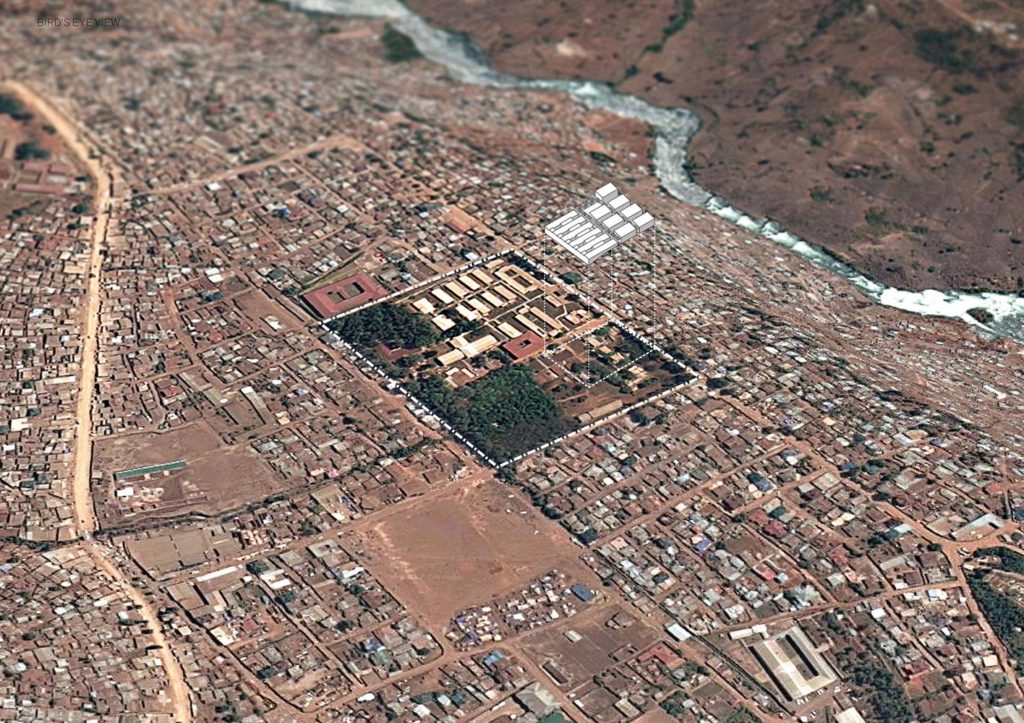
The hospital treats all kind of patients has become specialised in treating survivors of sexual violence. This care is based on a holistic person-centered care model covering medical, psychosocial, legal, and socioeconomic care needs. Maternal and neonatal care is a central part of the operations, with 3,000 to 3,500 childbirths per year.
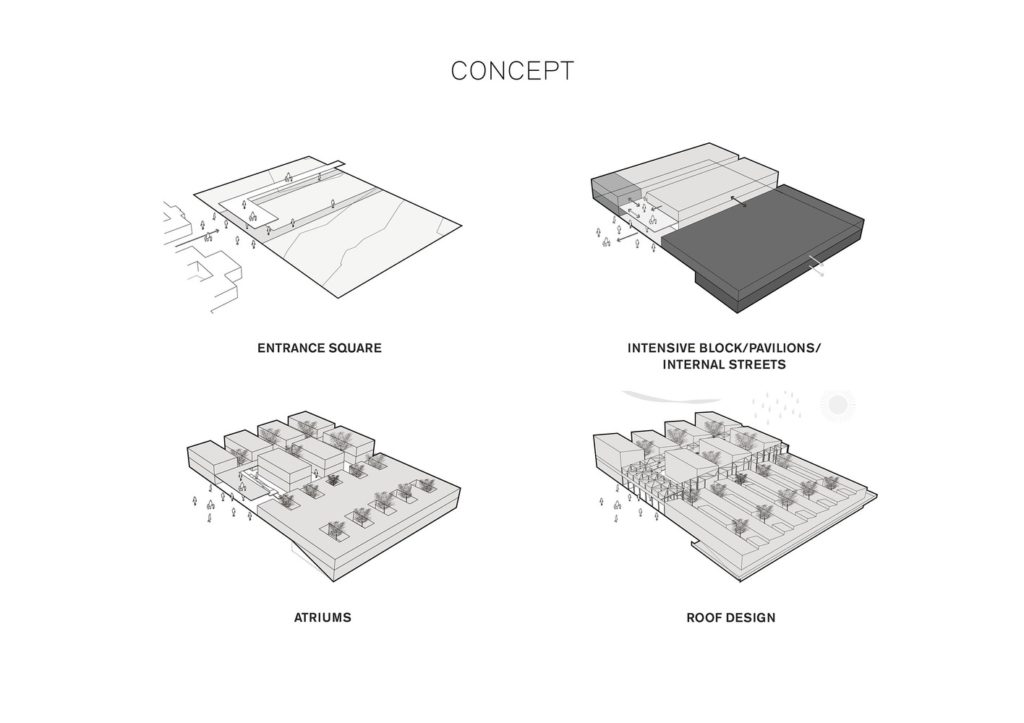
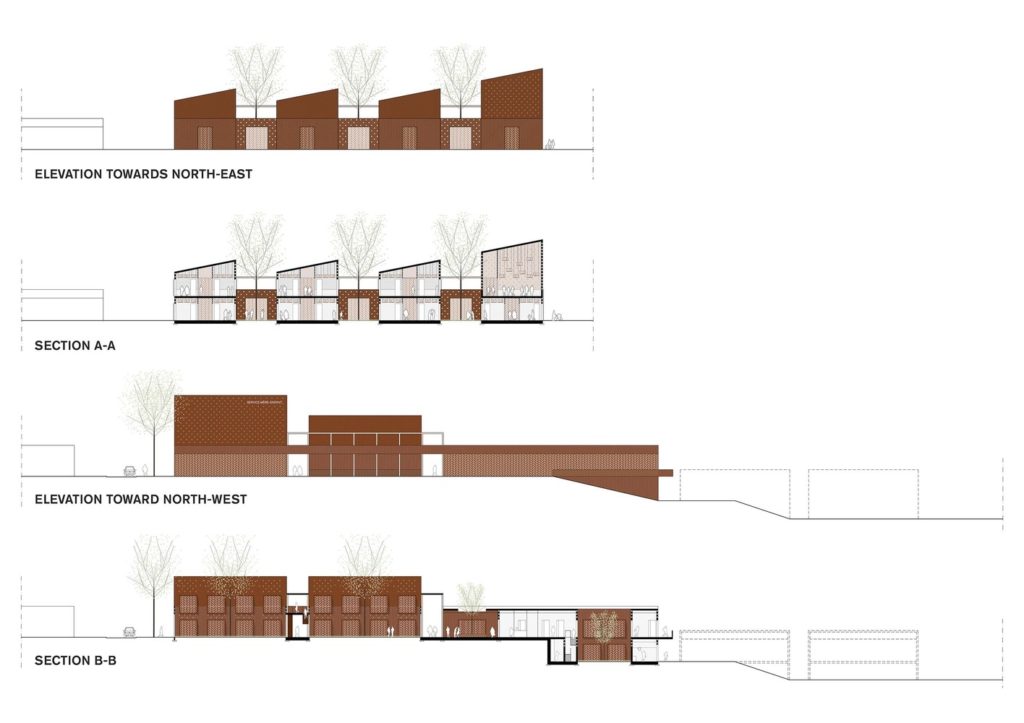

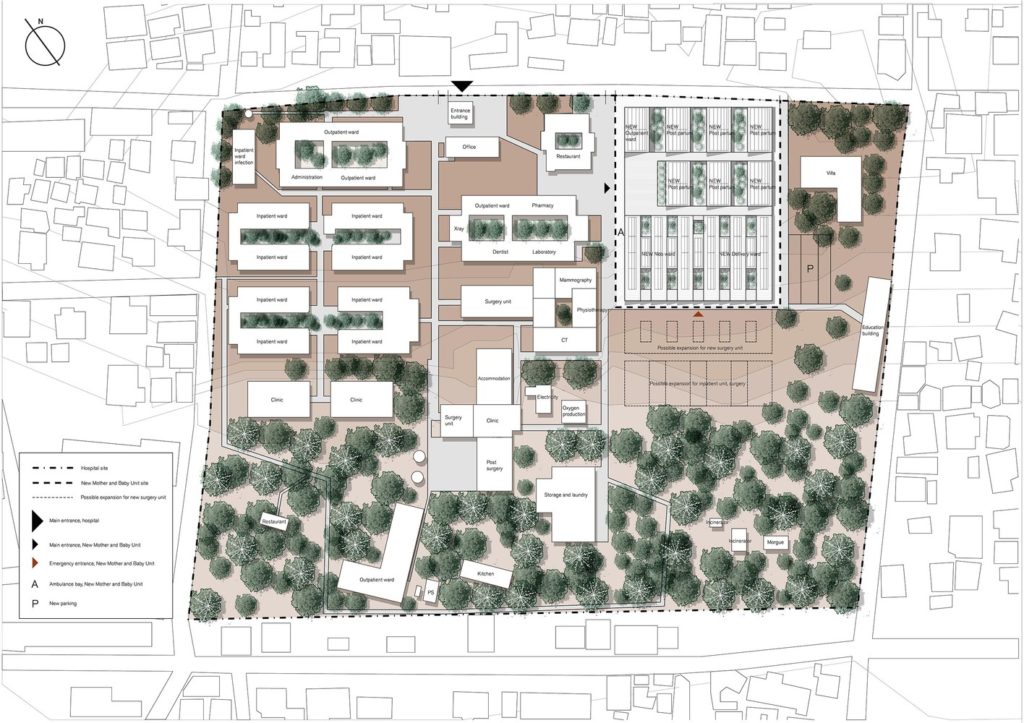
In close dialogue with the hospital’s management and staff, White, the University of Gothenburg, WSP, Art of Life and Birth and Chalmers Technical University have developed a concept for a centre where women can give birth accompanied by close relatives in a safe and professional environment. The unit is the first stage of a long-term masterplan, also developed by the team, which entails developing the entire hospital’s structure over the next 10-15 years. The unit is planned on the basis of on a scientific patient-centered holistic care philosophy and a healing architecture design.

In order to survey the operation’s needs but also to understand the site’s physical conditions, the existing buildings and the technical infrastructure, White visited the hospital. The study aims to verify the project’s feasibility with respect to the site’s limitations and also to define the building’s most important dimensions and overall appearance.
Developing a feasibility study of this type requires experience of designing healthcare buildings as well as experience of working in an international context. White has considerable experience and knowledge of building sustainably. The result is a design which minimises the hospital’s climate impact.

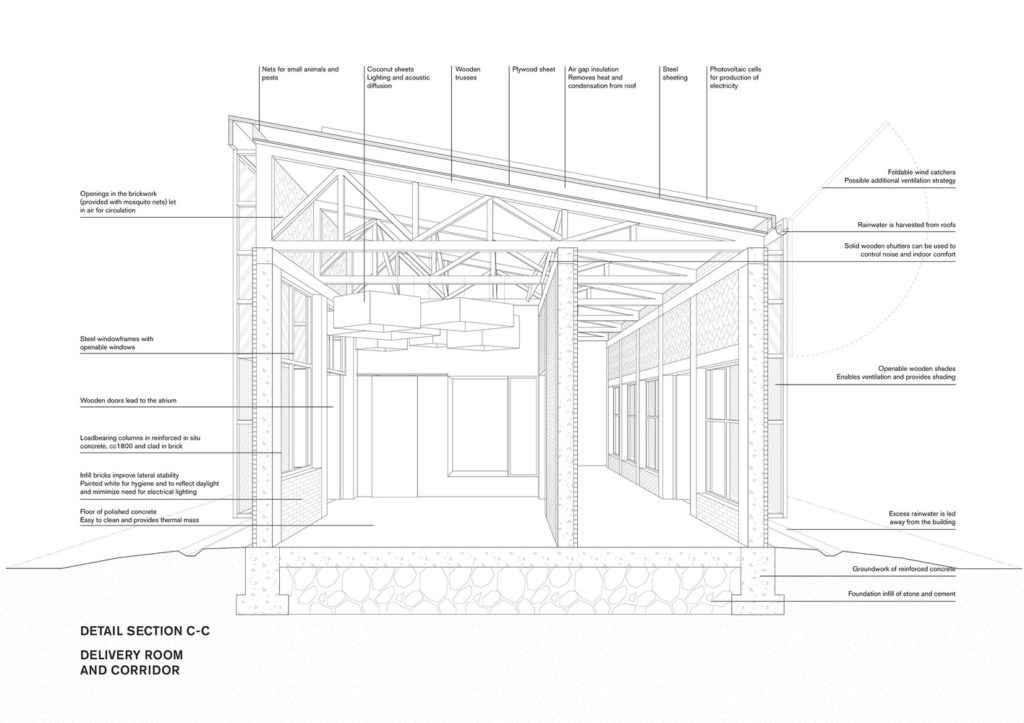
The roof is designed for optimum electricity and water supply, and bioclimatic design ensures a comfortable interior environment. Earthquake-proof modular buildings ensure long-term sustainable development and simultaneously ease maintenance.

The unit has been designed together with the hospital based on its working methods and needs. The design is also linked to the latest knowledge within evidence-based design. People’s desire for an attractive and welcoming environment, daylight, greenery, a private sphere and integrity is as strong in the Congo as in Swedish and Scandinavian projects; the feasibility study identified the need for a beautiful and welcoming environment with access to both private and social areas. Furthermore, abundant daylight, views over the natural environment and a comfortable indoor environment support the healing process. Navigating the hospital is also easy.

The response to the feasibility study was very positive, and White has been asked to continue working on the project in the next phase, followed by implementation together with local architects. In the long-term, the combination of White’s expertise and local knowledge can be developed into a concept which can be used in other places with similar conditions. The overall vision of the project is to develop a unit that can become a model for other maternity- and neonatal care health facilities in similar contexts in DRC, Africa and the world.

During our work on the feasibility study we have constantly been reminded that architecture can make a major difference. In the long term, we hope to be able to create a model to build healing architecture in developing countries rationally, sustainably and in an economically smart way.
Cristiana Caira, Lead Architect, White Architects





